Inflammatory Myopathy
Inflammatory Myopathy – Overview
Inflammatory myopathies are a group of rare, chronic muscle diseases characterized by muscle inflammation, weakness, and degeneration. These are autoimmune disorders, where the body's immune system mistakenly attacks its own muscle tissues.
1. Types of Inflammatory Myopathy
| Type | Description |
|---|---|
| Polymyositis (PM) | Affects mainly adults; causes symmetrical muscle weakness, especially in the shoulders, hips, and thighs. |
| Dermatomyositis (DM) | Similar to PM, but also involves a distinct skin rash. Can affect both adults and children. |
| Inclusion Body Myositis (IBM) | Affects older adults, involves slow progressive weakness in both proximal and distal muscles; less responsive to treatment. |
| Necrotizing Autoimmune Myopathy (NAM) | Characterized by muscle necrosis with minimal inflammation; often linked with statin use or cancer. |
| Juvenile Myositis | Affects children and includes juvenile forms of DM and PM. |
2. Causes and Risk Factors
-
Autoimmune reaction (most common cause)
-
Genetic predisposition
-
Infections (viral: HIV, HTLV, etc.)
-
Medications (statins, interferons)
-
Paraneoplastic syndrome (associated with cancers)
-
Environmental toxins
3. Symptoms
-
Progressive muscle weakness (usually symmetrical)
-
Difficulty rising from a chair, climbing stairs, lifting arms
-
Muscle pain or tenderness
-
Fatigue
-
Dysphagia (difficulty swallowing)
-
Shortness of breath (if respiratory muscles are affected)
-
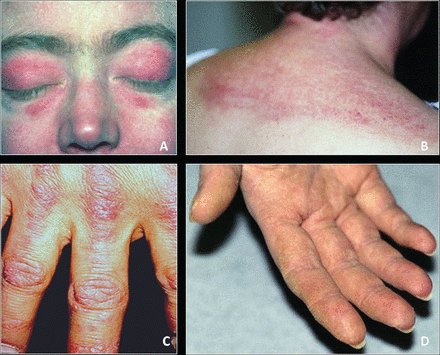
Rash (especially in dermatomyositis): heliotrope rash (eyelids), Gottron’s papules (knuckles)
4. Diagnosis
-
Physical examination and history
-
Blood tests: elevated creatine kinase (CK), autoantibodies (ANA, anti-Jo-1, etc.)
-
Electromyography (EMG)
-
Muscle biopsy (confirms diagnosis)
-
MRI: to detect inflammation in muscles
-
Skin biopsy (in dermatomyositis)
5. Treatment Options
Conventional (Allopathic)
-
Corticosteroids (e.g., prednisone) – first-line
-
Immunosuppressants (e.g., methotrexate, azathioprine)
-
IVIG (Intravenous Immunoglobulin)
-
Biologics (rituximab, especially in refractory cases)
-
Physical therapy – vital to maintain muscle function
Homeopathy (Supportive Use Only)
Note: No strong evidence supports homeopathy as a primary treatment. Always consult a qualified homeopath.
-
Rhus Toxicodendron – for muscle stiffness
-
Gelsemium – weakness with trembling
-
Causticum – for progressive paralysis
-
Arnica – muscle soreness
Ayurveda (Supportive Role)
Consult an Ayurvedic practitioner for personalized care.
-
Ashwagandha – improves strength and reduces inflammation
-
Guggulu – anti-inflammatory
-
Dashamoola – muscle rejuvenation
-
Abhyanga (oil massage) with Mahanarayan oil
-
Panchakarma therapies
6. Prognosis
-
Polymyositis & Dermatomyositis often improve with early treatment.
-
Inclusion Body Myositis progresses slowly and is less responsive to treatment.
-
Long-term outcomes depend on type, age of onset, and response to treatment.
7. Conclusion
Inflammatory myopathies are serious, autoimmune muscle disorders that require early diagnosis, specialist care, and long-term management. While conventional treatments are mainstays, supportive care through diet, exercise, physiotherapy, and traditional medicine may improve quality of life.