Guillain-Barré Syndrome
Guillain-Barré Syndrome (GBS)
Definition
Guillain-Barré Syndrome is an acute, rapidly progressive autoimmune disorder where the body's immune system attacks the peripheral nerves. It primarily affects the myelin sheath (the protective covering of nerves), causing inflammation and nerve damage that leads to muscle weakness and sometimes paralysis.
Causes
-
Often triggered by an infection, such as:
-
Respiratory infections (e.g., influenza)
-
Gastrointestinal infections (e.g., Campylobacter jejuni)
-
Viral infections (e.g., cytomegalovirus, Epstein-Barr virus, Zika virus)
-
-
Rarely triggered by vaccinations or surgery.
-
Exact cause unknown but involves immune system dysfunction.
Pathophysiology
-
Autoimmune response targets peripheral nerves.
-
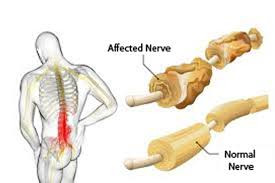
Demyelination (loss of myelin sheath) slows nerve signal transmission.
-
In severe cases, axonal damage (nerve fiber damage) occurs.
-
This leads to muscle weakness, sensory disturbances, and autonomic dysfunction.
Symptoms
Initial Symptoms:
-
Tingling or "pins and needles" in fingers, toes, or limbs.
-
Progressive weakness starting in the legs and moving upward (ascending paralysis).
Progression:
-
Symmetrical muscle weakness affecting legs, arms, and sometimes face.
-
Difficulty walking or climbing stairs.
-
Loss of reflexes.
-
Severe cases: paralysis of respiratory muscles requiring ventilation.
Other symptoms:
-
Pain or cramps.
-
Difficulty swallowing or speaking.
-
Autonomic symptoms: fluctuations in heart rate and blood pressure, sweating abnormalities.
Types of Guillain-Barré Syndrome
-
Acute Inflammatory Demyelinating Polyradiculoneuropathy (AIDP) – Most common form.
-
Acute Motor Axonal Neuropathy (AMAN) – Mainly affects motor nerves.
-
Acute Motor and Sensory Axonal Neuropathy (AMSAN) – Affects both motor and sensory nerves.
-
Miller Fisher Syndrome (MFS) – Rare variant characterized by ophthalmoplegia (eye muscle paralysis), ataxia, and areflexia.
Diagnosis
-
Clinical evaluation of symptoms and neurological exam.
-
Lumbar puncture: elevated protein with normal cell count in cerebrospinal fluid (albuminocytologic dissociation).
-
Nerve conduction studies: slowed conduction velocity, conduction block.
-
Blood tests to rule out other conditions.
Treatment
-
Hospitalization: Especially if breathing or swallowing is affected.
-
Supportive care: Respiratory support, physical therapy, pain management.
-
Immunotherapy:
-
Intravenous immunoglobulin (IVIG): Neutralizes harmful antibodies.
-
Plasmapheresis (plasma exchange): Removes antibodies from the bloodstream.
-
-
No cure, but most patients improve with treatment.
-
Recovery may take weeks to months; some may have lasting weakness.
Prognosis
-
Most patients recover fully or with minor deficits.
-
Some may have residual weakness or fatigue.
-
Early treatment improves outcomes.
-
Mortality is low but possible, mainly due to respiratory failure or complications.